
A blog of the Indo-Pacific Program
It seems that the United States often needs a crisis to force necessary change. After the Great Depression brought the United States to its knees in 1929, Franklin D. Roosevelt pushed the New Deal to provide a safeguard for millions of suffering Americans and created a social safety net that has been crucial to the financial stability of the American people ever since. After winning World War II, the United States created the CIA, the National Security Council (NSC), the Joint Chiefs of Staff, and the Department of Defense. While some may classify these large structural changes as government overreach, the reality is they were a stark display of lessons learned following a catastrophe.
The emergence and spread of COVID-19 provided the United States with a grim but unique opportunity to see the catastrophe coming, like beach-goers watching a tsunami slowly build until it finally, inevitably reaches them. Since the early days of the pandemic, when a novel pneumonia-like disease in Wuhan was first reported publicly, every country had the opportunity to learn lessons from those who were on the initial front lines of the pandemic. As the virus spread from nation to nation, first in those countries closest to China but eventually to countries like Italy and Iran, unaffected (to their knowledge) countries had to implement the strategies they have set in place for pandemic prevention. The United States was lucky enough to have a head-start to collect the information, data, and knowledge coming from affected countries to properly prepare for the inevitable.
Unfortunately, the U.S. failed to make use of this opportunity, and failed to heed the lessons that could have been learned from previous pandemics. This failure was made apparent through actions like defunding PREDICT – a government program tasked with finding viruses before they are introduced into the human population – and disbanding the global health security team on the NSC. As these failures grow more apparent and the number of confirmed U.S. cases and deaths continues to rise, in stark comparison to the relatively limited number of cases seen in parts of Asia, a range of explanations for these discrepancies have been offered.
Some point to culture as a driver of this dichotomy of successful responses in East Asia compared to failed responses in the United States and elsewhere in the West. They argue that Confucianism – which emphasizes duty to family and society over individual needs – explains the success of Asian responses while also excusing the failure of the West to do the same. Yet Taiwan and South Korea, for example, are both robust democracies with a strong history of opposing political authority – and their responses to COVID-19 have been exemplary. Nor, as this analysis demonstrates, have their effective responses to the coronavirus been founded on a greater degree of control or surveillance by the government.
Instead, an analysis of Asia’s successful responses to the coronavirus shows that most, though not all, of their actions are entirely replicable in the United States. Put simply, Singapore, Taiwan, and South Korea each were able to learn from the past, prepare for the future, and respond rapidly, decisively, and with great coordination in the early days of the outbreak. None of these are beyond the capacity of any functioning government, let alone the United States.
Learning the Lessons of SARS
Perhaps the most compelling and regionally-specific advantage Singapore, Taiwan, and South Korea had at the beginning of this crisis was of the shared memory and lasting impact SARS had on nations’ public health systems. For the U.S., SARS was a serious matter but did not result in lasting changes to its approach to pandemic preparation. Yet for the aforementioned countries of East Asia, SARS fundamentally changed their strategic calculus of pandemic preparedness on a national level.
In Singapore, SARS largely caught the public health systems off guard. After a “whole government approach” to fighting the virus, the public health systems were able to contain it by enacting more forceful measures like twice-daily temperature recording of medical professionals, constant surveillance of those quarantined, and effective strong communication all from the central government. Taiwan in the year following the SARS epidemic created the National Health Command Center (NHCC) in response to the glaring need to coordinate government powers on issues like bioterrorism and epidemiologic disaster mitigation and response. Similarly, South Korea, a country that has grappled with not only SARS but also MERS, another virus within the coronavirus family of which SARS is a member, established the Korea Centers for Disease Control and Prevention (KCDC). Like the NHCC, the KCDC was meant to consolidate the power of infectious disease response to a centralized source to unite the government against biothreats and compel the public to fall in line when the times call for it.
SARS also disproportionately affected health care workers, so the most innovative protocols that were established in its wake were focused on protecting the health care facilities themselves. In the face of COVID-19, Singapore implemented strict hospital guidelines around supplying, using, and cleaning personal protective equipment (PPE), delaying elective surgeries, and consistent and safe communication from hospital staff to officials and hospital administrators.
Taiwan instituted, among other policies, a ban on exporting masks, coupled with a ramping up of private Taiwanese mask production, and, to round it all out, a rationing system for mask procurement by the public to combat hoarding seen elsewhere. The uncertainty and surprising nature of SARS and MERS taught a lesson that time is a precious commodity during an outbreak. As a result, government action in concert with private industry was not considered as Plan B, but rather Plan A.
First Mover Advantage
Through their experiences with SARS, Asian public health experts also convinced their governments of the importance of acting quickly and decisively in the early days of a crisis. Without a rapid reaction, the disease can spread exponentially across a population and render containment impossible.
On December 31, 2019 – the same day China notified the World Health Organization that it had several cases of an unknown pneumonia – Taiwan’s CDC immediately ordered inspections of all passengers arriving on flights from Wuhan. Taipei was able to send a team of experts to the mainland on January 12, and while their trip was certainly state managed, the experts saw enough to convince their government to require hospitals to test for and report cases. Thus began Taiwan’s efforts to identify the infected and isolate anyone they had contacted – effectively containing the virus from rapid, exponential expansion. This all occurred before Taiwan confirmed its first case on January 21.
The South Korean government similarly acted quickly and decisively. Just one week after its first case was diagnosed in late January, government officials urged the private sector to mass-produce test kits. Within two weeks, thousands of test kits were being shipped per day even though at the time there were fewer than 100 confirmed cases. When an outbreak began in the city of Daegu, officials immediately began testing and contact tracing the infected.
Singapore similarly responded rapidly by quickly initiating massive testing and contact tracing programs while also restricting travel for people with a history of recent travel to China and parts of South Korea. In early February, it began a text and mobile web-based campaign to allow people under quarantine to report their location and instituted rules that anyone entering a government or corporate building in Singapore had to provide contact details to expedite potential contact tracing.
Testing: The Most Easily Fixed and Most Distressingly Botched
Timely, sufficient testing has been shown to be the most critical factor in disease containment and response. The process of testing the most people possible allows the government to understand the characteristics of the disease, grasp the gravity of the epidemic, and contain its spread by immediately isolating the infected and exposed. With COVID-19, the ability to aggressively test, trace, and track cases were critical to Singapore and Taiwan’s successes in keeping infection rates lower than anyone thought possible from the beginning – especially considering their proximity to, and connectivity with, the PRC.
South Korea had been equally successful in containing COVID-19 initially, but then faced a more chaotic situation with the infamous “Case 31:” a super spreader who attended two religious services and spread the virus at an alarming rate. But because of South Korea’s past experiences with SARS and MERS, Seoul was able to act quickly with a rapidly developed and approved test and then using the manufacturing power of its private industry to test at a massive scale – reportedly up to 20,000 tests per day. While this raised the publicly reported number of infected individuals, it also allowed South Korean health officials to effectively contain the disease through the tracking and tracing of the infecteds’ contacts. As a result, by March 17 South Korea had tested roughly 274,000 people while the US had only tested 41,000 at most – even though both countries reported their first case around the same time.
Looking ahead, COVID-19 should serve as a cautionary tale for the testing industry in the United States. Unfortunately, the flaws that lead to failures in testing were pluralistic with enough blame to spread between the regulatory hurdles of CDC and FDA, as well as the lack of NSC global health directorate to lead the process with executive authority. Perhaps the easiest change to make is by breaking precedent and considering adopting testing protocols that have been successfully used by other nations and endorsed by the WHO. Banking solely on the CDC’s record concerning testing will not serve us in the future. Global sharing or increased engagement with private industry from the start should be considered and instituted as soon as the dust settles from COVID-19.
The Power of the Private Sector
A key lesson that Singapore, Taiwan, and South Korea each learned from previous experiences was that private industry would be a critical player in meeting greatly intensified demand for PPE and other medical equipment, and established mechanisms for the rapid manufacturing of critical items. Taiwan quickly halted the exporting of all medical products and allocated resources – and even military personnel – to expand industrial capacity to produce medically necessary materials. By late January, Taiwan had stockpiled 44 million surgical masks, 1.9 million N95 masks, and 1,100 negative pressure isolation rooms and had expanded production of masks to 10 million per day. These would be vital resources for treating the infected and protecting healthcare workers.
Similarly, South Korea was able to quickly respond to the outbreak because of rapid cooperation between government and the private sector. In late January, with only four known cases, the South Korean government enlisted its private sector in rapidly developing tests, promising swift regulatory approval – which began to be granted one week later. Moreover, South Korea’s famous drive-through testing innovation was the result of government collaboration with the private sector: industry developed the drive-through idea, and government simplified the process of protecting medical workers.
Strong Centralized Government Power: A Unique Challenge for the U.S.
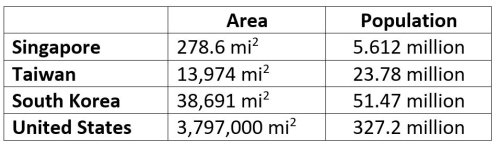
Beyond testing, the successes of Taiwan, Singapore, South Korea, and others in their initial response to COVID-19 stems from structural differences in the domestic distribution of power, making some aspects of Asia’s response to the pandemic difficult to replicate in the United States. The fact that the United States is geographically sizeable, with a much larger population, necessarily complicates any effort to implementing a cohesive and consistent public health response. Political and cultural aversions to large-scale, top-down government actions are prevalent across the country. Furthermore, state- and local-level officials simply have more power than the federal government to impose and implement the kind of strict social isolation policies necessary to limit the spread of disease. While there are certainly advantages to a decentralized approach to public health – for example, by making room for local governments to respond quickly to local threats — this approach poses a significant and unique obstacle to a nation-wide pandemic response.
Though these staggered processes of testing roll-outs, school closures, event cancelations, teleworking mandatory directives, localized curfews, and lockdowns may tip the scales in the heart and minds of those most fearful of centralized government action. Harkening back to the political effects of 9/11, the Great Depression, and the 2008 Financial Crisis, the federal government may have a chance to reform and consolidate in the wake of a catastrophe.
Moreover, the governments in Taiwan, Singapore, and South Korea each had the power to track the movements of its people and enforce quarantines to a degree that would be politically unfeasible in the United States. As of January 29, Taiwan announced it would electronically tracking individuals in quarantine (based on their travel from Wuhan) using GPS enabled government-issued cell phones to ensure individuals stayed within their specified boundaries or residences. Disobeying the quarantine would result in an enforced quarantine and potentially a fine. Cell phones would even be monitored for the amount of time the phone was stationary, to ensure people don’t circumvent the process by leaving home without their phone. Additionally, those under quarantine would have to be ready for irregular check-ins from authorities.
Even back in 2003, during SARS, Singapore’s government quarantined individuals and put them under police video surveillance to monitor their movements. With COVID-19, the CDC has sited compulsory, read as: legally enforced, quarantines for “asymptomatic close contacts” and “active monitoring” for contacts at a lower risk. Close contacts receive telephonic monitoring three times a day and those at lower risk, once a day. A contributor for Wired, Adam Rogers, recounts his sister-in-law’s updates from Singapore that, “everyone whose temperature is normal gets a sticker, and people are expected to acquire two or three stickers every day.”
Public Trust: Public Health’s Greatest and Most Tenuous Asset
While Asia’s response to COVID-19 demonstrates that rapid and massive testing, combined with a strong, centralized, and consistent approach to public health are necessary for an effective response, they are insufficient without public trust. Public trust is not gained through policy or a successful economy. Public trust is more abstract and relies on a government’s ability to appear credible, consistent, and transparent in its efforts to provide information, give advice, and act in the best interests of its citizens.
In recognition of this, Taiwan, Singapore, and South Korea each understood the whole-country response as untenable without the public’s confidence and instituted measures to keep their publics informed while maintaining consistent messaging across the government. In an analysis conducted by Human Rights Watch on global COVID-19 responses, a key section is included-- dubbed Protect freedom of expression and ensure access to critical information. Without adherence to these two key tenets, through actions like suppressing journalists and scientists, nations risk an “undermined trust in government actions.” Singapore, in particular, is highlighted in the analysis for publishing and regularly updating infection and recovery rates. Taiwan also made all relevant information surrounding COVID-19 easy to access and almost immediately held daily press conferences aimed to combat misinformation and provide transparency. South Korea gave twice-daily briefings from health officials and provided regularly updated public health data transparency.
Lessons Learned?
The failure of the United States in each of these categories directly contributed to the rapid spread of COVID-19 across the country. Whereas Asian countries learned from past experiences, tested early and massively, established trust with accuracy and transparency, empowered the private sector in the first days of the crisis, and responded quickly and decisively, the United States did not.
It is important to note that not all aspects of Asia’s responses are replicable in the United States. For example, it is inconceivable to imagine that the American people would ever allow the federal government to so blatantly track them with their personal electronic devices or imprison them for noncompliance with a quarantine. Here, is where no New Deal, no DoD, no re-jiggering of FDA requirements for testing that can help. This is likely an insurmountable obstacle to which U.S. public health officials will need to adapt.
This, of course, is only muddled by the abstract nature of public trust. A recent NPR/PBS NewsHour/Marist poll found that 60 percent of Americans have “Not very much” or no trust at all in the president’s information on COVID-19. The misinformation reported from the Press Briefing Room has prompted some media outlets to air their own fact-based analysis in place of the daily briefings and there have been calls from respected journalists to have the biggest cable networks do the same. The recorded lack of trust and mismatched messaging between public health officials and the executive branch only add obstacles to the critical whole-country approach fueled by the will of the people and the trust in their government.
The fundamental lesson to be learned from Asia’s response to COVID-19 is that each society must adapt its approach to its particular circumstances. Yet some principals are universal: they are dictated by the cold realities of epidemiology, and they do not wait or forgive unpreparedness, disorganization, or indecision.
Will this be the time when the United States finally learns the lessons that others in Asia had already learned? After COVID-19 passes into history, will the United States finally put into place the mechanisms, resources, and policies necessary to ensure that it is never again caught unprepared? Will a future leader be willing to risk the appearance of overreaction, of startling markets and the American people, in order to prevent the infection and death of thousands? To prepare for the next pandemic, the United States need not abandon its support of free market economics. It does not need to follow China’s practices of oppressive restrictions on movement and surveillance. Freedom and preparation can, and must, coexist. If the United States does not learn and heed these hard-earned lessons, the American catastrophe of COVID-19 is bound to happen again. Ultimately, the success of any response to a pandemic will rest on the government’s ability to act quickly and marshal sufficient resources, and on the ability and willingness of the American people to follow isolation guidelines.
Follow Alex Long, Program Associate for the Science and Technology Innovation Program (STIP) at the Wilson Center, on Twitter @w_alexlong.
The views expressed are the author's alone, and do not represent the views of the U.S. Government or the Wilson Center. Copyright 2020, Asia Program. All rights reserved.
Author


Indo-Pacific Program
The Indo-Pacific Program promotes policy debate and intellectual discussions on US interests in the Asia-Pacific as well as political, economic, security, and social issues relating to the world’s most populous and economically dynamic region. Read more


Hyundai Motor-Korea Foundation Center for Korean History and Public Policy
The Center for Korean History and Public Policy was established in 2015 with the generous support of the Hyundai Motor Company and the Korea Foundation to provide a coherent, long-term platform for improving historical understanding of Korea and informing the public policy debate on the Korean peninsula in the United States and beyond. Read more


Science and Technology Innovation Program
The Science and Technology Innovation Program (STIP) serves as the bridge between technologists, policymakers, industry, and global stakeholders. Read more





